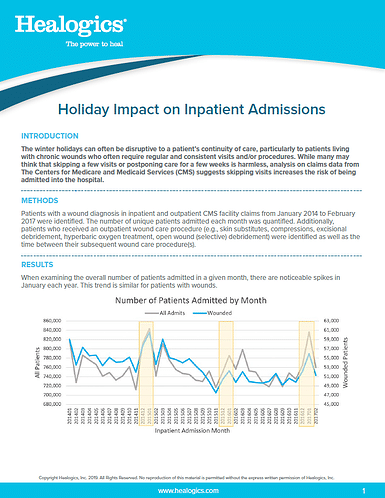
The winter holidays can often be disruptive to a patient’s continuity of care, particularly to patients living with chronic wounds who often require regular and consistent visits and/or procedures. While many may think that skipping a few visits or postponing care for a few weeks is harmless, analysis on claims data from The Centers for Medicare and Medicaid Services (CMS) suggests skipping visits increases the risk of being admitted into the hospital.
Learn More
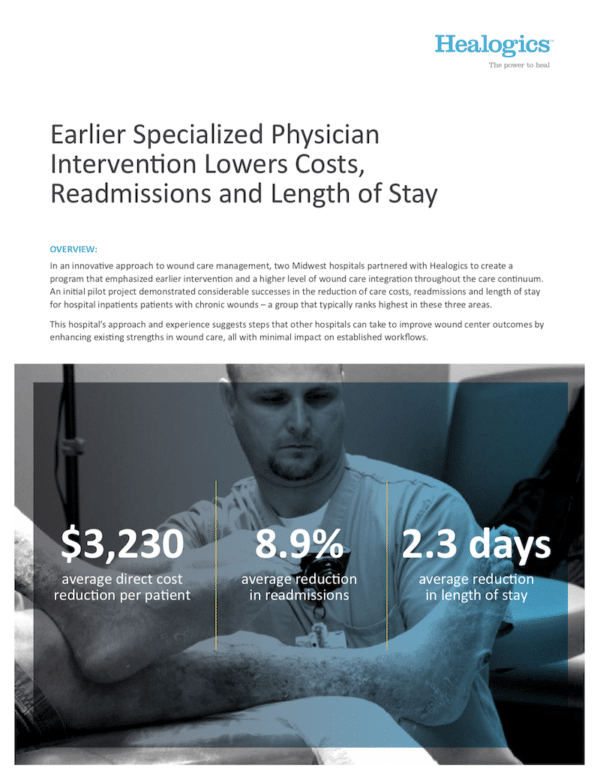
In an innovative approach to wound care management, two Midwest hospitals partnered with Healogics to create a program that emphasized earlier intervention and a higher level of wound care integration throughout the care continuum. An initial pilot project demonstrated considerable successes in the reduction of care costs, readmissions and length of stay for hospital inpatients patients with chronic wounds – a group that typically ranks highest in these three areas.
This hospital’s approach and experience suggests steps that other hospitals can take to improve wound center outcomes by enhancing existing strengths in wound care, all with minimal impact on established workflows.
Learn More
The findings of the study emphasize the importance of standardization and transparency in wound outcome reporting. However, while useful, until a standardized risk-adjustment methodology is applied, both the comprehensive and standard healing rates are necessary to understand the quality of care.
Learn More
Chronic wound patients face a number of challenges to their health and well-being. The presence of the ulcers is an indication of broader physical systems failures. However, with education and prevention, many wounds could be prevented or treated when they are less severe resulting in improved outcomes. The association between chronic conditions such as diabetes, cardiovascular disease, and social conditions is well established. Yet, none of the previous studies have addressed chronic ulcers. Healogics Wound Science Initiative is partnering with hospitals and researchers to better understand how the social determinants of health impact the lives of wounded patients.
Learn More
The Healogics Wound Science Initiative is a collaborative effort that aims to accelerate data-driven improvements, advance insights and perspectives, and identify mechanisms to continuously improve patient outcomes and reduce costs in the treatment of chronic wounds. The Wound Science Initiative is committed to using the Healogics data to guide the creation of wound outcomes measures that allow for industry-wide standardization and aggregate quality benchmarking.
Learn More
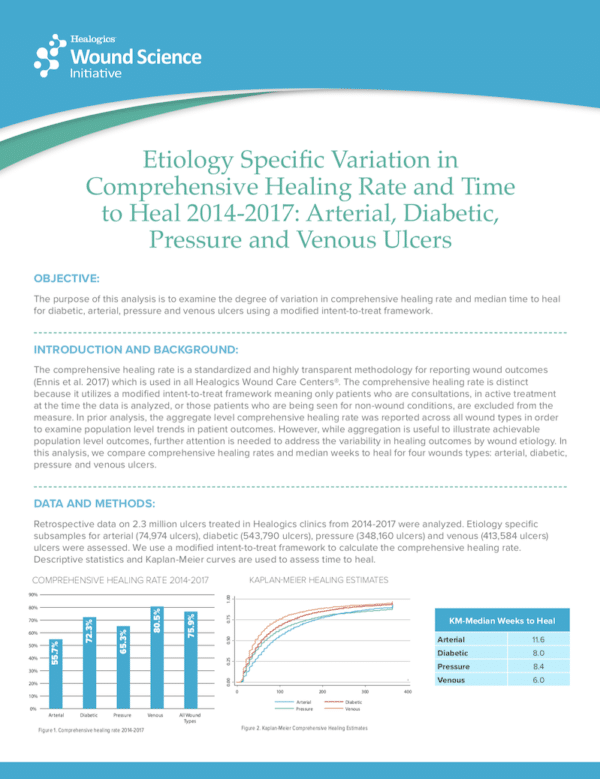
The purpose of this analysis is to examine the degree of variation in comprehensive healing rate and median time to heal for diabetic, arterial, pressure and venous ulcers using a modified intent-to-treat framework.
Learn More
HBOT increases the dissolved oxygen content in blood plasma. Functionally speaking, this translates into a systemic increase in reactive oxygen (oxygen free radicals) and reactive nitrogen species. The direct result includes a number of physiological benefits to the wounded host.
Learn More
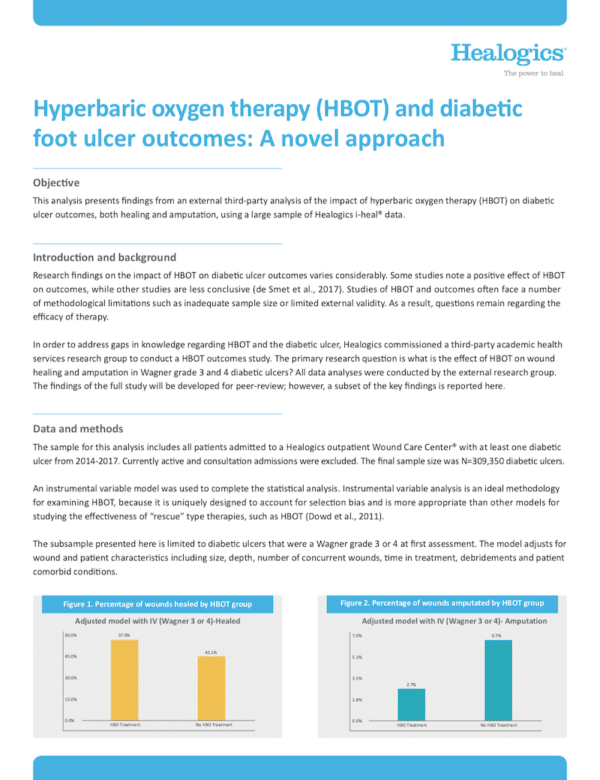
This analysis presents findings from an external third-party analysis of the impact of hyperbaric oxygen therapy (HBO) on diabetic ulcer outcomes, both healing and amputation, using a large sample of Healogics i-heal® data.
Learn More
Quality of Care Would you send your mother or father to your wound care center? How many of your patients are getting healed and in how long? Efficiency, Cost and Utilization Is your wound center profitable? How productive is your current staff compared to national benchmarks? Are you using wound care supplies and consumables effectively?…
Learn More