Healogics on Innovations in Medicine by PBS
William J. Ennis DO: Historically, when people think about, “what is a wound?” In general, they think immediately about the elderly, they think about bed sores, nursing homes, pressure ulcers. But interestingly, 6.7 million people in the U.S. suffer from a non-healing wound at any one point in time. There is over 50 billion dollars spent on healthcare dollars in the U.S. alone on this issue. There’s a marked increase in the number of patients with diabetes. There’s an aging population, and there’s an epidemic of obesity. All three of those factors make the prevalence of wound care anticipated to grow 2% per year over the next 5-10 years. It’s about surgical incisions that don’t heal. It’s about chronic diseases that have skin manifestations. People with diabetes have foot ulcers. 25% of all diabetics will have a foot ulcer in their lifetime. And so, it’s a prevalent disorder that requires a specialized center to care for.
These patients are complicated. Often times they require physical assistance to get out of their wheelchair and get in an exam room. It requires massive numbers of overhead, such as staff, people, special skills, special equipment. Primary care can’t provide that type of care.
Narrator: Specialty physician, Dr. Russel Dounies, tells us what makes this wound care center special.
Russell Dounies, MD: This is a phenomenal staff. Our case managers, our nurses, our receptionists. They’re just phenomenally good, and that is what actually brought me here. And there is nothing in this world that is better than working with competent people who care about what they’re doing and are constantly striving to do the best they can.
Narrator: Dr. Ennis outlines the various treatment modalities at a wound care center.
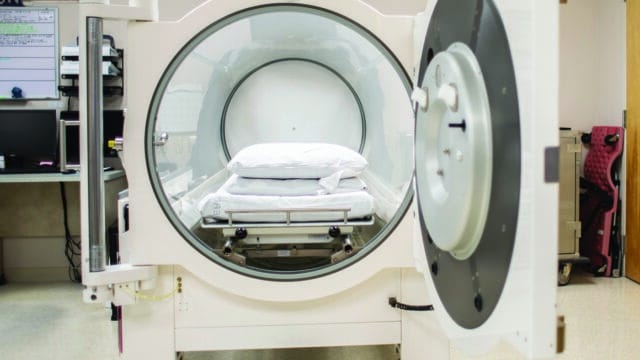
Dr. Ennis: When a patient comes to a center, a wound care center, what should they expect? What things are going to happen there differentially than maybe in your primary care office? Those things are, for example, surgical procedures, debridements, removal of tissue that needs to be removed in order to expedite the healing process. Special graphs, biologicals, there is an entire field of new devices being created to accelerate wound healing. Negative pressure wound therapy, biomechanical devices, and hyperbaric oxygen for patients that fail standard care and other types of methods. Wound care is not, “what dressing do I put on”, it’s, “how do I medically manage the patient in or der to heal their wound.”
Narrator: Treatment guidelines ensure the best outcomes for patients.
Dr. Ennis: One of the things that we utilize in our wound care centers is something called CPGs or Clinical Practice Guidelines. These are nothing more than the best evidence, recommendations for providers to utilize on all patients. What it does, is it eliminates unnecessary variation in care. It ensures that no steps are dropped off. You know, think of it like a checklist in the cockpit of an airplane. You know, I don’t care how many times the pilot has flown my flight, I really want that person to look through that checklist. Just to make sure nothing got dropped off. And that’s really what a clinical practice guideline does. It allows us across all of these centers to deliver as consistent as possible, healthcare for a wide diversity of patients with a wide number of wound ideologies.
Narrator: Research and technology have yielded better options for patients and increased healing rates.
Dr. Ennis: So, one of the innovations that has occurred in the past 5-10 years in the field of wound care, is the growth of product development and cellular-based and tissue-based products. So, these are devices and dressings, if you will, that are implanted into a patients non-healing wound that can completely restart the healing process. They come from a myriad of locations, so, amniotic membrane is being used. Animal tissue is being used. Human cadaver skin is being used. And all of these things are utilized to supplement the patient who has some type of inherent problem in healing their own wound. It’s almost like a jump start. The cells actually can invigorate the patient’s own tissue by the release of growth factors to almost get back to a natural healing course.
Narrator: Patients have had remarkable results due to the care they received at a wound care center.
Loretta Tinker: If I hadn’t gone to the wound care center and got the care that I needed, I don’t believe that I would have a foot to walk on today. Um, it’s that big of a difference and I’ve still got my balance. I’m going to be able to go back to my job. Um, I’m going to be pretty much back to normal.
Narrator: With the resources of a national network of wound care centers, Healogics is able to build a database of patient information for over one million wound treatment plans, and their outcomes, which is used to determine the best treatment course for each patient. We continue now with Dr. William Ennis. He tells us how this data facilitates better patient care.
Dr. Ennis: At Healogics, we really pride ourselves on data, outcomes, and translating that data and outcomes to better patient care.
Dr. Dounies: You combine all the information from all the clinics that are run by the Healogics corporation. That gives you a phenomenal database. Now somebody goes through and they sort that out and they form the clinical practice guidelines. And they say this is what was done, this is what worked, these are the things to consider. So, you have all of that information available that you don’t if you’re on your own.
Dr. Ennis: So, using big data techniques, we can roll that information up and we can determine things like, what is the healing rate across the country for overall wounds, and then for more specifically, a patient with sickle cell anemia who is greater than 25 years of age, who maybe has some type of other social determinance of health issues. What’s their chance of healing? And you really can’t do that out of a single hospital or even a single university. You really need the power of data, and the power of data is really in the aggregation of that data. And Healogics, I think, is second to none in that.
Value-based health is really different than volume-based healthcare of the past. So, we need to not only know that we’re going to get somebody healed, we need to know in how long and for how much money.
Narrator: The wound science initiative seeks to expand the news of better wound treatment to patients and the healthcare community.
Dr. Ennis: The wound science initiative at Healogics is a collaborative effort amongst providers, regulators, researchers. And the goal and objective is to disseminate information to not only the people that work in or centers, but nationally raise the level of education and knowledge about wound care, what options are available, and what you can expect when you come to a wound care center.
Narrator: An integrated team at the wound care center is committed to the best patient outcomes.
Dr. Ennis: When you’re in a specialized clinic that does nothing but focus on one disease entity, wounds, it requires more than one person. No one individual could possibly have the expertise required to handle one patient that has rheumatoid, one patient that has sickle cell, and a pressure ulcer on the same clinic day. That’s the beauty of an integrated team. So, having nurses, physical therapists, and physicians for multiple specialties and backgrounds all coming to the patient, rather than the patient trying to navigate that healthcare landscape and make all those appointments on themselves, that’s where you really get differential outcomes.
Arnold Demasters: I feel that a wound center is extremely important, because there, they know how to deal with that wound. With any wound, without having had the specialty of the wound center, it would be hard for me to realize what would have happened because I had already spent seven days, so to speak, with someone who wasn’t a part of a wound center without that knowledge and expertise.
Narrator: Dr. Ennis relates what he sees in the future of medicine and wound care.
Dr. Ennis: We believe that there’s going to be a tremendous increase in the treatment of patients in their own homes with the use of telemonitoring, telementoring, and telemedical devices. We also are already seeing an explosion of the use of apps. Where patients are going to be doing some self-monitoring. We think there’s going to be a tremendous change in who comes to the wound clinic, and certainly who goes to the hospital. We think the future is going to be to allow us to really stratify that depending on their needs and their acuity, and technology is going to drive that.
In 2018, Healogics worked alongside PBS to create a 10-minute segment on wound healing featured on Innovations in Medicine. Viewed by an audience of over 100 million, Innovations in Medicine is a televised health series that explores the latest in research and treatments across the country.
In our segment on wound healing, Healogics Chief Medical Officer Dr. William Ennis discusses the growing population of people living with chronic wounds and why advanced wound care is so important in the ever-changing healthcare landscape. This segment also touches on Healogics Wound Science Initiative and how we are working hard to increase the science, awareness and practice of wound care.