This study presents a modified intent-to-treat framework for measuring wound outcomes and measures the consistency of population based outcomes across two distinct settings. In this retrospective observational analysis, we describe the largest to date, cohort of patient wound outcomes derived from 626 hospital based clinics and one academic tertiary care clinic. We present the results of a modified intent-to-treat analysis of wound outcomes as well as demographic and descriptive data.
Learn More
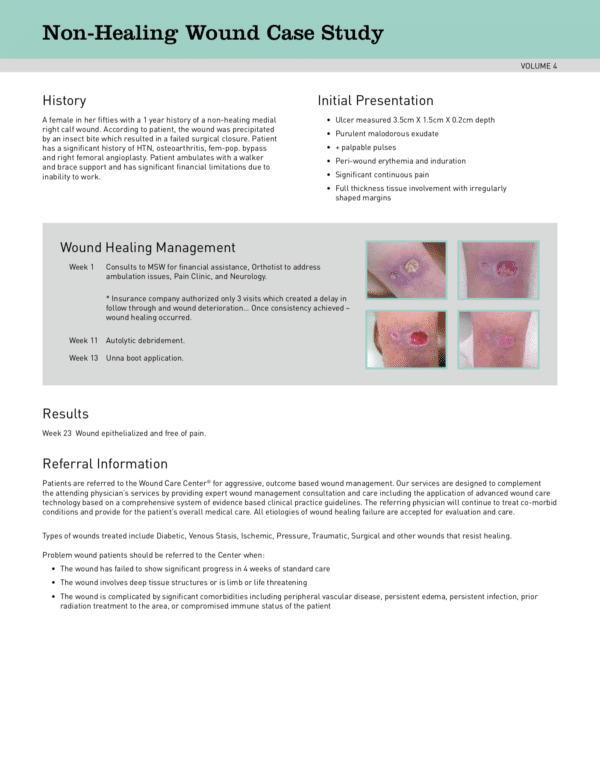
A female in her fifties with a 1 year history of a non-healing medial right calf wound. According to patient, the wound was precipitated by an insect bite which resulted in a failed surgical closure. Patient has a significant history of HTN, osteoarthritis, fem-pop. bypass and right femoral angioplasty. Patient ambulates with a walker and brace support and has significant financial limitations due to inability to work.
Learn More
The prevalence of lower extremity venous disease in our population is greater than that of peripheral arterial occlusive disease, although the latter receives more attention. An estimated 35 percent of the adult population has lower extremity venous abnormalities and one-fifth of these individuals will acquire one or more venous ulcers in their lifetime.
Learn More
Comprehensive wound management requires a provider driven, multi-disciplinary based program that directs critical resources required for evaluation and treatment to patients suffering from wound healing failure.
Learn More
To advance insights and perspectives on how to better manage the care of patients with chronic wounds and to stimulate potential solutions for improving outcomes and reducing
costs for this vulnerable, majority 65+ population, Healogics analyzed 2014 Centers for Medicare & Medicaid Services (CMS) Part A and B standard analytic files for care utilization and cost trends. This white paper synthesizes information and insights gleaned from the analysis, keeping in mind potential areas of opportunity to improve care and outcomes.
Learn More
Healogics researchers partnered with Dr. Alexandra Nowakowski, a leading patient advocate and medical researcher at Florida State University’s College of Medicine, to investigate provider perceptions of wound care. Healogics providers were recruited to participate in an anonymous nine-question survey focused on their experiences and perceptions of wound care and wounded patients. The questions focused on patient attributes that influence positive or negative wound outcomes, patient impacts on providers’ care plan and providers’ perspective of patient-centered wound care.
Learn More
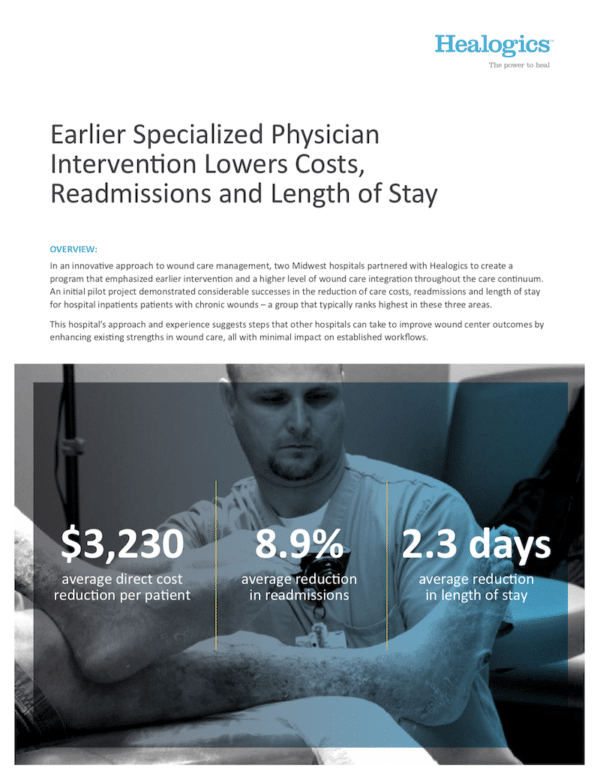
When two Midwestern hospitals partnered with Healogics to establish a new wound center, it was an opportunity
to address issues common to chronic wound care. While hospitals typically do a very good job of dressing wounds, wound centers do not typically engage with patients beginning with admission, and wound care management does not typically follow the patient post-discharge. This suggests opportunities for improvement.
Learn More
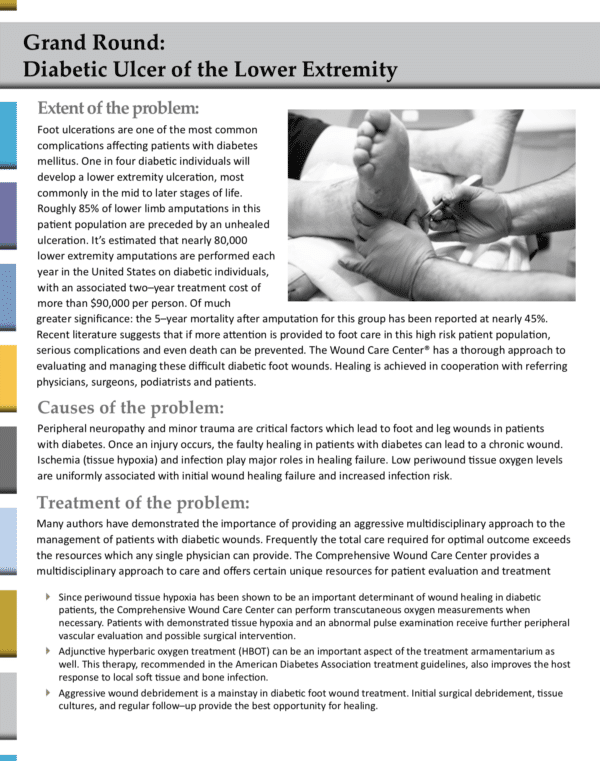
Foot ulcerations are one of the most common complications affecting patients with diabetes mellitus. One in four diabetic individuals will develop a lower extremity ulceration, most commonly in the mid to later stages of life. The Wound Care Center® has a thorough approach to evaluating and managing these difficult diabetic foot wounds. Healing is achieved in cooperation with referring physicians, surgeons, podiatrists and patients.
Learn More
The goal of this research was to identify a population of diabetic foot ulcer patients who demonstrate a significant response to hyperbaric oxygen therapy (HBOT) using a large sample size to provide guidance for clinicians when treating these complicated patients.
Learn More
Although diabetes can ravage the body in many ways, non-healing ulcers on the feet and lower legs are common outward manifestations of the disease. Also, diabetics often suffer from nerve damage in their feet and legs, allowing small wounds or irritations to develop unnoticed. Given the abnormalities of the microvasculature and other side effects of diabetes, these wounds take a long time to heal and require a specialized treatment approach for proper healing.
Learn More