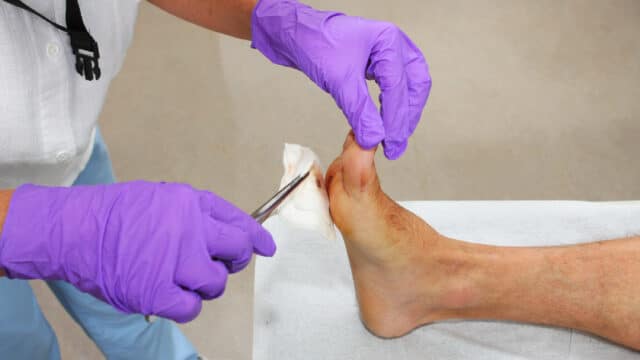
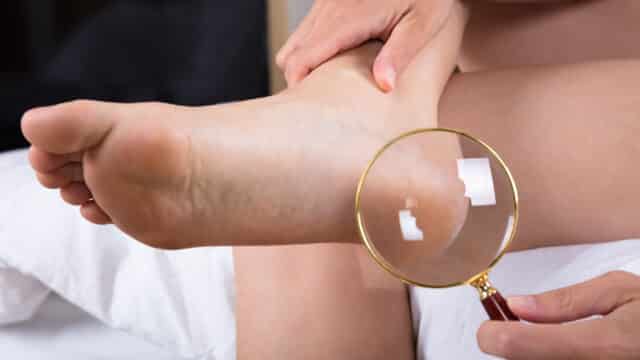
Understanding Diabetic Neuropathy and Foot Ulcers
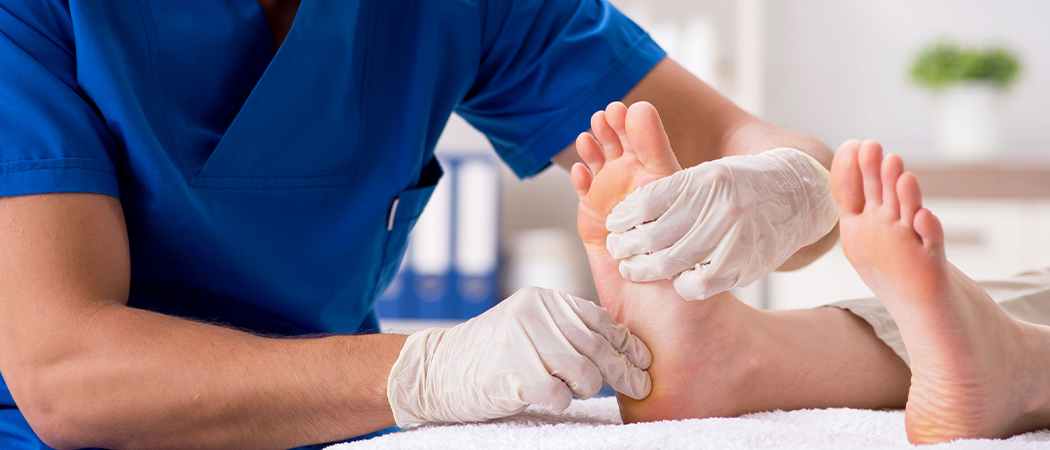
Diabetes affects over 37 million Americans, and with it comes a serious but often overlooked complication: diabetic neuropathy. This nerve damage condition may affect up to half of all people with diabetes, making it one of the most common diabetes-related complications. Yet many people don’t realize they have it until significant damage has already occurred.
Why This Matters: Diabetic neuropathy is the leading cause of non-traumatic foot ulcers, and non-healing diabetic foot ulcers account for up to 85% of diabetes-related amputations. However, with proper understanding, daily care, and early intervention, most of these serious complications can be prevented.
At Healogics, our mission to FIND. TREAT. HEAL.™ is rooted in compassion and is the foundation of our commitment to the communities we serve. We recognize the challenges of living with diabetes, particularly with complications like neuropathy and foot ulcers, which can significantly impact your quality of life. We are here to help you understand complications like diabetic neuropathy that can cause chronic wounds and foot ulcers.
What Causes Diabetic Neuropathy?
Diabetic neuropathy is a common complication of diabetes that we often see in our patients. It occurs when high blood sugar levels damage blood vessels, reducing their ability to deliver blood to nerves. This leads to nerve damage, typically affecting the lower legs, feet, and toes.
We know it can be concerning to experience a loss of sensation or feeling in your feet. Without the protective feeling of pain, even a small wound might go unnoticed. That’s why we emphasize the importance of regular foot checks – even the smallest wound could develop into a diabetic foot ulcer (DFU) if left untreated.
Understanding Diabetic Foot Ulcers
A diabetic foot ulcer is a wound that we commonly see on the ball of the foot or toes of our patients who have diabetes. These ulcers often begin as calluses, which tend to occur more frequently and build up faster on diabetic feet due to high-pressure areas under the foot.
If you notice that calluses are forming on your feet, it might be a sign that you need therapeutic shoes and inserts. It’s important to manage calluses because if left untrimmed, they can become very thick, break down, and eventually form diabetic foot ulcers.
If left untreated, these ulcers can grow larger and deeper— another complication of damaged blood vessels and poor circulation. When oxygen-rich blood doesn’t reach the wound, it can’t heal properly. This can lead to infection, hospitalization, and, in severe cases, amputation. That’s why education, prevention, and early intervention are so important.
We have prepared this patient-education download to help you learn the steps to prevent diabetic foot ulcers.
Recognizing Neuropathy Symptoms
We often hear from our patients about symptoms like tingling, weakness, and numbness in their feet, which can be signs of neuropathy. If you’re experiencing these symptoms, we want you to know that we can help. Our caring healthcare providers use a simple, painless test to diagnose neuropathy, which can be done at any of our Wound Care Centers.® We gently tap nerves on your feet and legs with a thin plastic wire to determine the severity of any nerve damage.
While neuropathy can’t be cured, we can work together to prevent further damage. We’ll guide you on improving circulation and teach you how to check for potential wounds every day.
The Importance of Early Intervention
At Healogics, we’re dedicated to raising awareness about the importance of screening and early intervention. Did you know that non-healing diabetic foot ulcers account for up to 85% of diabetes-related amputations? That’s why we’re here to help you take proactive steps in your foot care.
The Power of Early Action:
Why Timing Matters:
- Early-stage ulcers heal faster and with fewer complications
- Prompt treatment can prevent minor problems from becoming major ones
- Regular monitoring catches issues before they become serious
- Professional intervention provides access to advanced treatments
What Early Intervention Includes:
- Immediate assessment of any foot problems
- Professional wound care using advanced techniques
- Pressure offloading to allow healing
- Infection prevention and treatment when needed
- Patient education on ongoing prevention
- Coordination with your diabetes care team
Don’t let concerns about foot ulcers or neuropathy hold you back from the activities you love. Take the first step towards better health today – reach out to your nearest Healogics Wound Care Center® for a consultation—no referral needed! Click here to find a location near you!
Frequently Asked Questions
How do I know if I have diabetic neuropathy?
Early signs include tingling, burning, or numbness in your toes and feet. However, neuropathy can develop without noticeable symptoms. Regular screening with your healthcare provider, including simple tests like the monofilament test, can detect neuropathy before you notice symptoms.
Can diabetic neuropathy be reversed?
While nerve damage from neuropathy cannot be completely reversed, excellent blood sugar control can slow or stop progression. Some people experience improvement in symptoms with better diabetes management, though this varies by individual.
How often should I check my feet?
You should inspect your feet every single day, preferably at the same time, so it becomes a habit. Use good lighting and a mirror if needed, or ask someone to help you check areas you can’t see easily.
What should I do if I find a small cut on my foot?
Clean the cut gently with mild soap and water, apply an antibiotic ointment if recommended by your healthcare provider, and cover with a sterile bandage. Contact your healthcare provider the same day to report the injury, even if it seems minor.
Are there special shoes I should wear?
If you have neuropathy or foot deformities, therapeutic diabetic shoes may be recommended. These are specially designed to reduce pressure points and accommodate foot changes. Many insurance plans cover diabetic shoes when prescribed by a healthcare provider.
How can I improve circulation in my feet?
Regular physical activity (as approved by your healthcare team), maintaining good blood sugar control, not smoking, and elevating your feet when sitting can all help improve circulation. Avoid tight socks or shoes that restrict blood flow.
What’s the difference between a callus and an ulcer?
A callus is thickened skin that forms in response to pressure or friction. An ulcer is an open wound or sore. Calluses can break down underneath and develop into ulcers, which is why proper callus management is important.
Should I be worried about every foot problem?
While not every minor issue becomes serious, people with diabetes and neuropathy should take all foot problems seriously. What might be minor for someone else can become a major problem when you have reduced sensation and healing ability.
Expert Care at Healogics
At Healogics, we understand that managing diabetic neuropathy and preventing foot complications requires specialized expertise and ongoing support. Our wound care specialists are trained in the latest evidence-based approaches to diabetic foot care and prevention.
Take Control of Your Foot Health Today: Don’t wait for problems to develop. If you have diabetes, especially with any signs of neuropathy, proactive care is your best protection. Contact Healogics today to schedule a comprehensive foot evaluation and learn how to protect your feet for life. Click here to find a location near you!